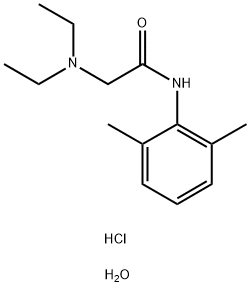
Linocaine hydrochloride is a white or almost white, crystalline powder with slightly bitter and numbing taste. Soluble in water, ethanol and organic solvents, insoluble in ether. The aqueous solution does not decompose under acid and alkali conditions, and it rarely deteriorates after repeated autoclaving.
Linocaine hydrochloride is a fast voltage-gated sodium channel blocker that used in Local anesthesia and heart rhythm disorders. Its actions are more intense and its effects more prolonged than those of procaine but its duration of action is shorter than that of bupivacaine or prilocaine.
Anesthetic (local); antiarrhythmic (class IB). Long-acting, membrane stabilizing agent against ventricular arrhythmia. Originally developed as a local anesthetic.
ChEBI: Linocaine hydrochloride is the monohydrate form of lidocaine hydrochloride. It is a local anesthetic and cardiac depressant used as an antiarrhythmia agent. Its actions are more intense and its effects more prolonged than those of Procaine but its duration of action is shorter than that of bupivacaine or prilocaine.
Alpha caine Hydrochloride (Carlisle); Anestacon (Polymedica);
Laryng-O-Jet (International Medication); Lidocaton (Phar maton); Lidopen (Meridian); Xylocaine (Abraxis); Xylo caine (AstraZeneca); Xylocaine (Dentsply).
Linocaine hydrochloride is an anesthetic of the amide group, like articaine or bupivacaine. Immediate-type IgE-dependent reactions are rare, and delayed-type contact dermatitis is exceptional. Cross-reactivity between the different amide anesthetics is not systematic.
Lidocaine Hydrochloride is the hydrochloride salt form of lidocaine, an aminoethylamide and a prototypical member of the amide class anesthetics. Lidocaine interacts with voltage-gated Na+ channels in the nerve cell membrane and blocks the transient increase in permeability of excitable membranes to Na+. This prevents the generation and conduction of nerve impulses and produces a reversible loss of sensation. Lidocaine hydrochloride also exhibits class IB antiarrhythmic effects. The agent decreases the flow of sodium ions into myocardial tissue, especially on the Purkinje network, during phase 0 of the action potential, thereby decreasing depolarization, automaticity and excitability.