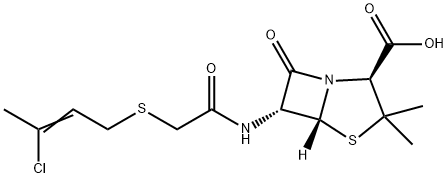
The original fermentation derived penicillins were produced by growth of the fungus
Penicillium chrysogenum on complex solid media, with the result that they were mixtures differing from one
another in the identity of the side-chain moiety. When a sufficient supply of phenylacetic acid is present in
liquid media, this is preferentially incorporated into the molecule to produce mainly benzylpenicillin
(penicillin G in the old nomenclature). Use of phenoxyacetic acid instead leads to phenoxymethyl penicillin
(penicillin V). More than two dozen different penicillins have been made in this way, but these two are the
only ones that remain in clinical use. The bicyclic penicillin nucleus itself is prepared biosynthetically via a
complex process from an acylated cysteinyl valyl peptide.
Bacteria may exhibit resistance to penicillins and other
β-lactam antibiotics by several mechanisms :
? Acquisition of penicillin-binding proteins (PBPs)
with reduced affinity for penicillin. This is a frequent
cause of resistance in Gram-positive bacteria such
as staphylococci, pneumococci and enterococci.
This mechanism may also be responsible for lowlevel
penicillin resistance in H. influenzae and viridans
streptococci.
? The production of a bacterial enzyme, β-lactamase, that
opens the β-lactam ring, causing inactivation of the antibiotic.
? Modification of outer membrane proteins (porins) in
Gram-negative bacteria, preventing passage of penicillins
into the bacterial cell. Efflux mechanisms have been
described in which bacteria pump out β-lactam antibiotics.
Bacteria frequently display more than one resistance
mechanism
– for example, methicillin-resistant staphylococci
typically produce β-lactamase but demonstrate resistance primarily
due to altered PBPs; Gram-negative bacteria may
produce β-lactamases in organisms with efflux mechanisms
or altered outer membrane proteins.
Methicillin-resistant strains of Staphylococcus aureus
(MRSA) are considered to be resistant to all β-lactam antibiotics,
with the exception of some newer cephalosporins,
and are frequently multiresistant. The prevalence of MRSA is
variable, with very low incidence in some countries of northern
Europe, but high incidence in Japan and other countries.
In the USA the frequency increased from 2.4% in 1975 to
64% in 2007. Although largely confined to hospitals, MRSA
is increasingly seen in community settings.
When benzylpenicillin was introduced, all streptococci
were sensitive to its action, and this situation remains largely
unchanged. However, pneumococci exhibiting reduced susceptibility
are now common, although the criteria for penicillin
resistance differ in the USA and Europe .
The interpretive criteria for non-meningitis isolates defined
by the FDA in 2008 is based on clinical experience showing
that high doses of penicillin provide efficacious drug concentrations,
except in cerebrospinal fluid (CSF). The EUCAST
or FDA pre-2008 definitions are generally used for epidemiological
purposes.
Until the 1980s, clinical isolates of Streptococcus pneumoniae
were uniformly susceptible to penicillin, except for a few
reports from South Africa and elsewhere. By 1998, 24% of
invasive pneumococci isolated in the USA displayed reduced
susceptibility to penicillin and often to other classes of antibiotics.
The frequency of isolation of penicillin-resistant pneumococci
in Europe was 51% in Hungary (1990) and 9% in the UK (1998). Introduction of the heptavalent pneumococcal
vaccine in 2000 caused a dramatic decrease in isolates
of pneumococci insusceptible to penicillin, especially in the
elderly and young children, in countries with effective vaccination
programs.
As with pneumococci, enterococci were initially perceived
always to be susceptible to ampicillin and benzylpenicillin, but
resistant strains are now common. Resistance is less prevalent
among the most common species, Enterococcus faecalis, in which
β-lactamase has been reported at a low frequency. In Enterococcus
faecium, the next most common enterococcal species, high-level
penicillin resistance due to modified PBPs is usual.
Veterinary Drugs and Treatments
Natural penicillins remain the drugs of choice for a variety of bacteria,
including group A beta-hemolytic streptococci, many grampositive
anaerobes, spirochetes, gram-negative aerobic cocci, and
some gram-negative aerobic bacilli. Generally, if a bacteria remains
susceptible to a natural penicillin, either penicillin G or V is preferred
for treating that infection as long as adequate penetration
of the drug to the site of the infection occurs and the patient is not
hypersensitive to penicillins.
Veterinary Drugs and Treatments
Penicillins have been used for a wide range of infections in various
species. FDA-approved indications/species, as well as non-approved
uses, are listed in the Uses/Indications and Dosage section for each
drug.